How Gynecology Visits Change Throughout Your Life - Page 8
Share the post
Share this link via
Or copy link
A lot of individuals are wondering whether or not they should go in for routine physical exams during the COVID-19 pandemic. According to news reports, many doctors are conducting routine exams using Telehealth portals, seeing most patients through their computer screens, and only recommending in-person visits in certain cases. Meanwhile, research shows that Americans have missed hundreds of thousands of important cancer screenings due to the pandemic. Naturally, there is a lot of anxiety over going to any sort of medical office right now. Medical facilities are where sick people go – right? Not necessarily.
As for specialists, they’re following CDC guidelines for things like screening patients and only allowing in so many people at a time. And on the topic of specialists, women should not skip their gynecology visits during this time. A woman’s body goes through significant changes every decade, and sometimes in a matter of just a couple of years – you know, about the length of a pandemic. We decided to speak to a gynecologist about what doctors in her medical field look for during each phase of life. Dr. Shrusan Gray of women2womenobgyn.com lent her knowledge for this piece.

Source: 3PM Media / 3PM Media
When do women start going to GYN visits?
Dr. Gray explained that the right age for a young woman to start visiting a gynecologist is entirely subjective. “It’s a no judgment type of deal. We take care of our patients as far as what their needs are…I always tell moms, ‘If your daughter isn’t yet 21 and isn’t sexually active, she can see a regular doctor. She doesn’t need pap smears or cultures or STD testing.” But as soon as women become sexually active, Dr. Gray says a gynecologist should become involved in their care to discuss things like STD prevention, and taking care of their bodies in this new phase of life.

Source: SDI Productions / Getty
When visits become regular
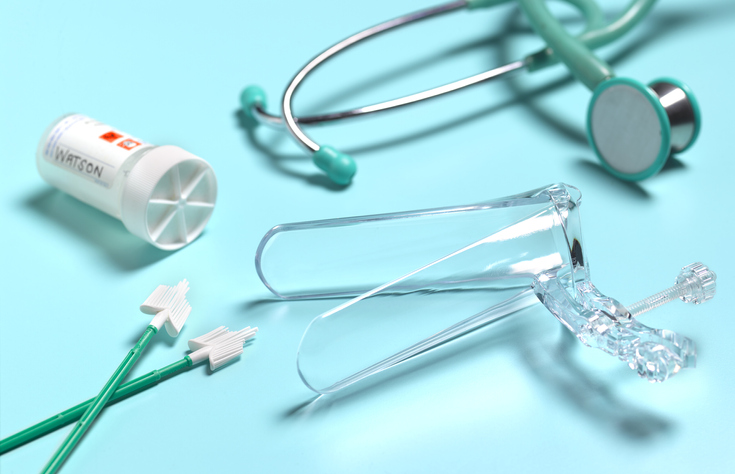
“By 21 we hope everybody shows up to their gynecologist. There are additional discussions to be had. Whether it’s in regards to cervical cancer screening and vaginal screening or what’s normal and what’s not normal,” says Dr. Gray. “Females are always curious about what’s normal in appearance as far as their discharge, or about things they might be feeling that they might not think is normal like odors, itching, and so on.”
Source: Peter Dazeley / Getty
When pap smears begin
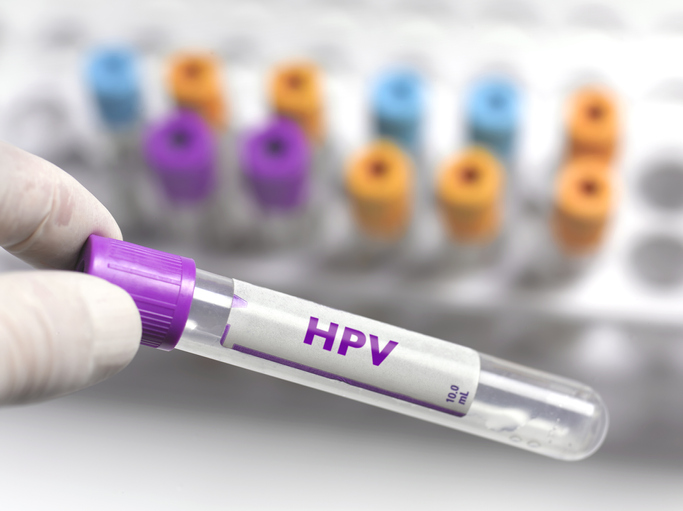
“We start screening for cervical cancer or abnormal paps at age 21. It usually depends on what the pap smear looks like that determines if HPV testing is done,” says Dr. Gray. And she adds that she isn’t necessarily testing for every type of HPV. “We are testing for high risk versus low risk. We test for high risk because those are the ones that can cause cervical cancer and are involved in changing the cells on your cervix. That testing can start as early as 21 based on what the cells look like when you do a pap smear.”
Source: Peter Dazeley / Getty
Testing for HPV in your 20s and 30s
“By the time you get to your late 20s or 30s, we are doing HPV testing as a baseline. But it can change. Maybe at 21 you had an abnormal test and an HPV test that was positive. After that, you might always get an HPV test. The HPV test shows you if the HPV virus is active. Generally, a lot of us gynecologists think that 70 to 80 percent or more of patients who are sexually active – especially if you have multiple partners who have multiple partners – have already been exposed to HPV.”

Source: sturti / Getty
When is HPV a concern?
“I reassure patients with an abnormal pap that HPV is pretty much a part of the norm. It’s a very common aspect of life. The question is whether or not it’s affecting your cervical cells – the cells that line your cervix or vagina,” explains Dr. Gray. “The low-risk HPV viruses, which are not usually tested for, are viruses that don’t cause as much damage as far as likelihood of causing cervical cancer. They can cause genital warts. But people aren’t usually worried about warts if they aren’t presenting.”

Source: MicroStockHub / Getty
How often should you get screened?
There are conflicting views on how often a woman in her 20s or 30s should receive pap smears, especially after an irregular one. “If you’ve had an abnormal pap smear, I err on the side of what makes the patient comfortable,” says Dr. Gray. “If you’ve had an abnormal one, you should err on the side of getting screened every year. Even if you’ve had normal pap smears for a while. That might be how I differ from other gynecologists. I feel patients are uncomfortable not being evaluated on a yearly basis after an abnormal pap smear.”

Source: kate_sept2004 / Getty
When it’s time to talk fertility
Along with cervical cancer screenings, fertility will be a thing your gynecologist should discuss with you when you enter your 30s, says Dr. Gray. “Entering 30s, you’re asked if you want kids. Now, with women having careers and full lives, we get busy. Before you know it, you’re flying through your 20s and then your 30s. You don’t realize that your fertility is not indefinite. A lot of women do not realize how definite our fertility is.”

Source: LumiNola / Getty
What are your options?
“Some physicians assume of patients ‘If they want babies, they’ll talk to me.’ A lot of women don’t realize how important it is to talk about family planning in terms of how much time we have left to have healthy pregnancies and what sorts of conditions our bodies must be in to have healthy pregnancies. It is a conversation that is necessary when women enter their thirties.”

Source: Ana Rocio Garcia Franco / Getty
What about single women who want kids?
Dr. Gray emphasizes that as a physician, there is no judgment. But she wants to be clear on what her patients want, and help them understand their options. If they’re in their 30s and want kids, she asks “Are they married? No? If you don’t know if you’ll have a mate, let’s discuss the preservation of the eggs, which is not as expensive as we think it is. It could be a viable option for a lot of women out there… Some women say ‘My grandma got pregnant at 45.’ Okay, but how many women really get pregnant at 45?” Being aware of the real statistics is important, says Dr. Gray.
Source: kali9 / Getty
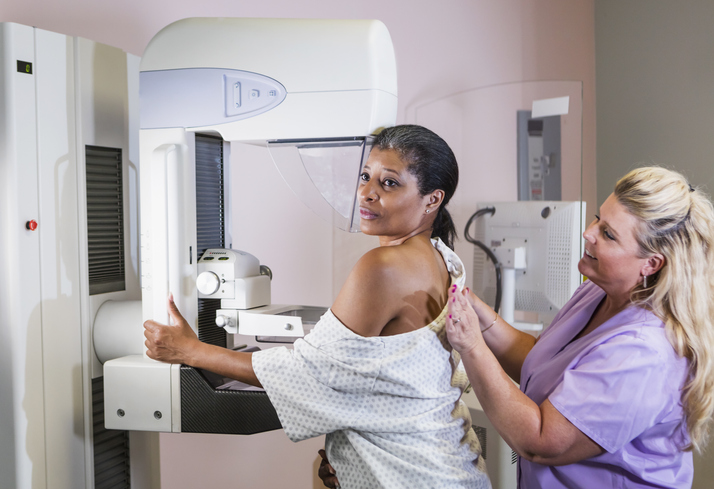
Screenings in your 40s
“When you hit your mid to late 40s, gynecology visits are very important. This is when a lot of women see gynecological diseases and start to go through hormonal changes like menopause and perimenopause. There can be too heavy or irregular periods. It could be fibroids or other reasons. Most women by the age of 40 have fibroids,” explains Dr. Gray.

Source: FatCamera / Getty
How prevalent are fibroids and what are they?
“Fibroids are smooth muscle tumors which are benign, but they do cause significant symptoms. They grow large. They cause heavy bleeding and pain. This can happen in the 20s and 30s but the 40s is the most common time. Sixty percent of women by their 40s have some form of fibroids, from tiny ones to large ones.”

Source: Grace Cary / Getty
Another painful condition
“Endometriosis can come up. This is when we have endometrial cells that line the uterus – the ones that come off during your period – found outside the uterus. Either on the ovaries or on the bowels. Sometimes in the GI tract. Prior to periods, it can be very painful. Imagine having your period, and having some symptoms even worse, because it’s not just happening at the uterus.”

Source: FatCamera / Getty
Talking about the big M
“Then there is menopause and post-menopause. The hormonal changes. The hot flashes. The night sweats. In post-menopause, some women in their 60s and 70s still have menopausal symptoms,” states Dr. Gray. “But then they have body changes like increased weight gain and vaginal changes. Urinary symptoms. Overactive bladder. One major thing is vaginal dryness and painful intercourse. It’s a pretty common issue for women of that age and it’s really difficult for them.”

Source: Carol Yepes / Getty
Why GYN visits always matter
If you don’t need an annual pap or have finished menopause, you may feel you don’t need to see your GYN regularly. But Dr. Gray reminds us that gynecologists perform many important exams that your primary physician does not. If someone skips their GYN visits, Dr. Gray warns, “Then that person does not get evaluated for breast exams. Their physician may not do breast exams. So who is doing the breast exam? Who is looking in the vagina? Who is feeling your uterus and your ovaries? If someone has a new sexual partner, who is doing the STD screening? There is way more to a GYN exam than a pap smear. A female needs a GYN exam every year. Just like you see a primary care doctor every year.”

Source: Coolpicture / Getty
Other life-long screenings
At any age, “It’s important to talk diseases that are common,” says Dr. Gray. “By 40 years old we’re ordering mammograms for women. Unless they have a high risk, then earlier. Fibrocystic breasts are things we take care of. And we’re screening for cancers like ovarian cancer. Some patients are at high risk like those with predispositions in their family history. We’ll do the genetic screening.” Genetic screening can happen at any age, says Dr. Gray, and is determined by the age at which the family member with the history was diagnosed, along with other factors.
-

Bucket Baddies With Big Energy — The 30 Hottest NBA Players In The Game Right Now
-

The Black Estate: Meet Quincy and Tawian Livingston — The Atlanta Couple Redefining Black Homeownership
-

Not Just Sex—14 Signs He’s Not Just Sleeping With You, He’s Falling For You
-

A Whole Gallery Of Fine — The 30 Sexiest Black Men Who Dominated 2025








