Here's What African Americans Need To Know About Hepatitis C
Hepatitis C: What African Americans Need To Know About The Liver Disease

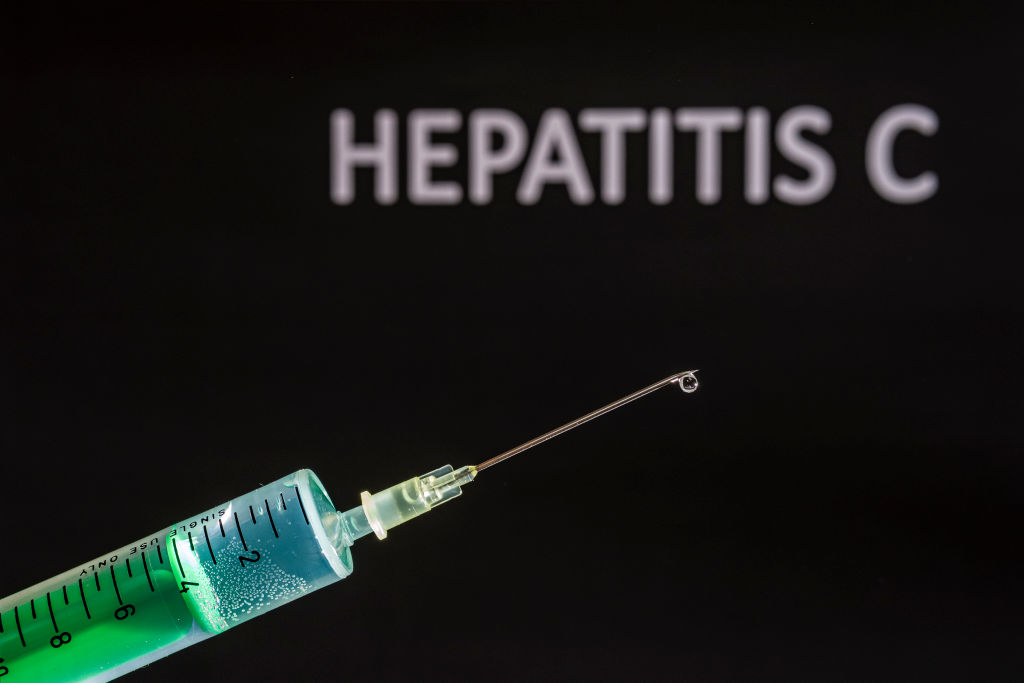
Hepatitis C virus. | Source: BSIP / Getty
Originally published on News One
Nearly 33 years ago, a collective of scientists leading research at a biotechnology firm nestled in Emeryville, California unearthed the existence of the hepatitis C virus (HCV). Since that ground-breaking discovery was made, the condition has spiraled into becoming the deadliest infectious disease in America.
For the Black community, the systemic racial inequities that pervade the country’s healthcare system have exacerbated its detrimental impact. Research shows African Americans are twice as likely to be infected with hepatitis C in comparison to the general U.S. population and were less likely to be treated for the virus. Over the past few decades, measures have been taken to promote early detection and improve the responsiveness of medical treatments for people of color, however, changing the narrative starts with awareness.
THE ORIGINS OF A SILENT PROGRESSIVE DISEASE
Hepatitis C is classified as a virus that triggers infections of the liver. It’s primarily transmitted through exposure to blood containing the virus. According to the Centersfor Disease Control and Prevention, hepatitis C encompasses an infection spectrum spanning from mild to long-term illness. Acute hepatitis C is a short-term illness that occurs within the first six months of transmission. Symptoms include jaundice—which is defined as yellowing of the skin—urine and stool discoloration, nausea and pain in the upper right abdomen. When detected early, it can significantly reduce the risk of chronic infection.
Chronic hepatitis C lies on the long-term side of the spectrum and in many cases can serve as the prelude to liver and bile duct cancer. The form of the virus progresses in silence as many people may not experience symptoms for decades until they develop complications from liver scarring. Studies show more than half of individuals who contract hepatitis C will develop a chronic infection.

Grammy Award winner Natalie Cole speaks about hepatitis C at the National Press Club in Washington, D.C. in 2011. Cole was diagnosed with the disease in 2008. | Source: Stephen J. Boitano / Getty
The groups that are most vulnerable to the virus include individuals with HIV infection and those who share needles or other devices to inject drugs. Babies born to mothers who carry the virus can contract it during delivery. Healthcare workers run the risk of infection as well since they are subjected to needlestick injuries in the workplace.
Smaller transmission risks include sexual contact with an individual infected with hepatitis C, sharing personal items—like razors and toothbrushes—that may be exposed to blood contamination and getting tattoos and piercings in uncleanly spaces. Individuals who have undergone blood transfusions or organ transplants before 1992 are also at risk of infection due to complexities surrounding blood screening methods decades ago.
Dr. Alana Biggers, an ABMS board-certified internal medicine physician who also serves as an assistant professor at the University of Illinois at Chicago College of Medicine, told NewsOne that the amplification of information related to the virus is the key to saving lives.
“Spreading awareness is very important because it’s another preventative measure,” shared Dr. Biggers. “The recommendations have changed over the last couple of years or so. When I first started as a physician the recommendation was for people within the war baby generation to get screened for hepatitis C, but then looking at the data they were seeing that young people were also getting hepatitis C brought mostly by the opioid crisis that’s been going on over the last couple of decades. If you’re an adult, you should get screened at least once in your lifetime. If you are somebody who uses injection drugs or any other type of paraphernalia you should get screened more often.”
When it comes to the diagnosis and treatments for hepatitis C, the playing field is far from level. Although some progress has been made in relation to the creation of culturally-responsive medical treatment, African Americans are the most at risk and have a significantly higher rate of infection and mortality from hepatitis C and its relative issues.
ROOT CAUSES OF HEPATITIS C’S RACIAL DIVIDE
Similar to other viruses and diseases Americans are grappling with, hepatitis C is not omitted from disproportionately and devastatingly affecting the Black community. A study revealed African Americans account for about 20 percent to 23 percent of diagnosed hepatitis C infections despite being just 13 percent of the U.S. population. In 2019, chronic liver disease was among the leading cause of mortality among Black people between the ages of 45 and 64 years old.
When it comes to matters of accessibility to treatment, socioeconomic barriers can define an individual’s fate. Dr. Biggers shared the reasons for the disproportionate impact are multifactorial. “These reasons include lack of health insurance leading to lower access to healthcare, lower screening rates, and less access to doctors who treat hepatitis,” she told NewsOne. “Additionally, Black communities are twice as likely to be uninsured or have Medicaid. The treatment options for hepatitis C are more likely to be denied by Medicaid insurers. Lack of access to healthcare can lead to lack of access to proper treatment.” Dr. Biggers also noted African Americans have historically been deemed ineligible for hepatitis C treatments without a viable reason as they have the same risk factors as anybody else. She believes combatting discrimination and bias within the healthcare system will shift the alarming trends.
Source: Frank Bienewald / Getty
The disparities don’t stop at trying to get a foot in the door for life-saving treatment. Historically, there have been racial gaps in responsiveness to medicine. Studies show while other racial groups typically reach a sustained virological response after eight weeks of treatment, African Americans typically need 12 weeks. Further research revealed that 87.8% of Black people achieved SVR12 in comparison to 92.4% of white people.
Over the past few years, medical innovation has been a driving force in creating equitable, effective and efficient treatments. “Some of the earlier medications for hepatitis C were generally bad. They weren’t really curing many people at all, and it seemed like it was even worse in the African American community,” shared Dr. Biggers. “There are new direct-acting antivirals that can cure hepatitis C in over 90% of people. The cure rates are the same regardless of race or ethnicity with the new antiviral medications.”
ADVANCEMENTS IN PREVENTION AND THE CALL FOR EQUITY
Extensive research centered on treatment and health outcomes has contributed to the advancement of solutions to help individuals navigate hepatitis C. HCV is curable when treated with a newer antiviral medication.
“People take these medications for 8-24 weeks or typically 8-12 weeks,” said Dr. Biggers. “If a person has liver damage from scarring, known as cirrhosis, or previous treatments for hepatitis C, the doctor will also check the virus genotype—a type of hepatitis C infection—to determine the length of treatment.”
She added there are several preventative steps one can take to avoid contracting hepatitis C including not sharing needles, other drug equipment or personal items and getting tattoos or body piercings in clean environments from professionals who use sterile tools and unopened ink. She also stressed the importance of wearing gloves if you come in contact with someone else’s blood or open sores.
Health professionals like Dr. Biggers and others who are using their platforms to evoke transformative change within medicine are contributing to a collective awareness of hepatitis C and its effects. Overall, she believes reversing the staggering impact hepatitis C has had on communities of color begins with early diagnosis. “People should make sure they are tested for hepatitis C,” she shared. “Getting a diagnosis early can lead to better treatment options that can help to cure hepatitis C.”
SEE ALSO:
My Brother’s Keeper: Black Communities Need To Speak More Openly About Their Health
Multiple Myeloma Is A ‘Silent Killer’ Of Black People
[ione_media_gallery id=”3053899″ overlay=”true”]












