The Different COVID-19 Tests Explained, Plus At-Home Testing Mistakes
The Different COVID-19 Tests Explained, Plus At-Home Testing Mistakes You Should Be Aware Of
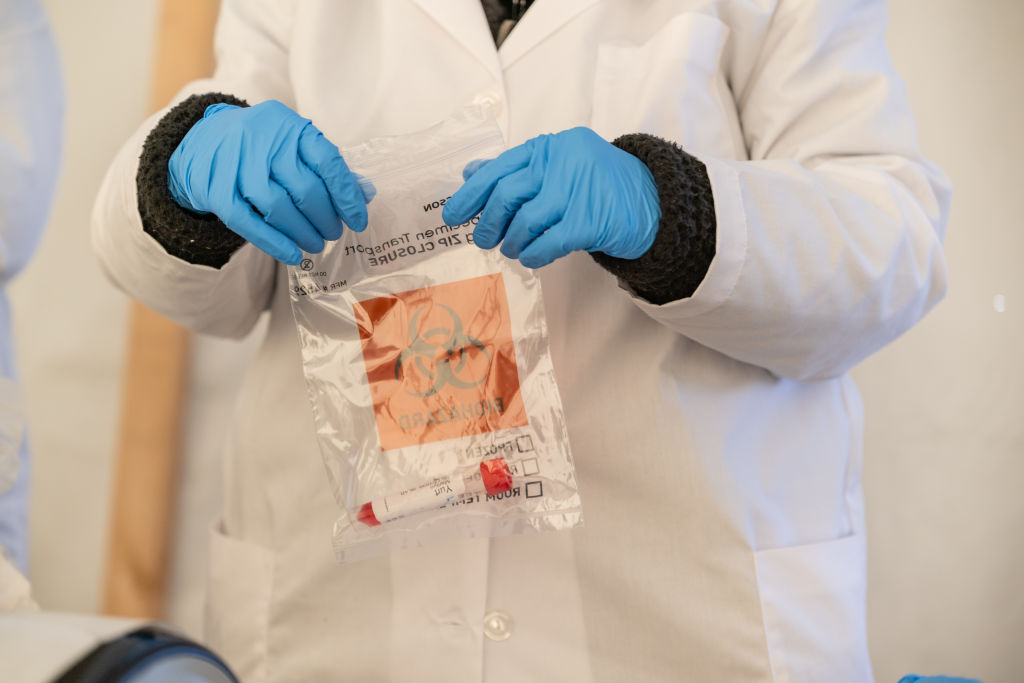
Source: Jon Cherry / Getty
Viral. Rapid. PCR. At-home. There are so many different COVID-19 test types. Most people have probably received a couple of different kinds of tests by this point, not fully knowing the ways each one varies in accuracy or how they work. Still, as people are eager to get tested, they should know. One New York Times piece tells of families spending hundreds of dollars in a matter of months on at-home COVID-19 tests. The County of Los Angeles Public Health shows a recent spike in testing, as well as new cases.
A lot rides on the results of COVID-19 testing. Things like whether or not you can get on a flight, attend that dinner party, visit that relative or show up for that work opportunity. We make big decisions – decisions that could impact the health of others – all based on what these tests say. So there’s value in understanding them and using them wisely. Here’s a look at the different COVID-19 test types and ways you might be at-home testing incorrectly.
Viral Tests

Source: Jackyenjoyphotography / Getty
When looking into COVID-19 tests, you’ll often find two options: Viral and Antigen. Viral tests check to see if an individual is currently infected with COVID-19. They are diagnostic tests. They’re typically collected through a sample of mucus or saliva that is collected from the nose – either the back or the middle of the nose – and are sometimes taken from inside of the cheeks, the tongue, the throat or the gums. Within viral tests, there are two subcategories of tests: molecular (also called PCR) and antigen. A molecular test looks for the RNA found inside of the virus. The antigen test looks for the proteins found on the surface of the virus. Yale Medicine reports that molecular tests are generally the more accurate of the two tests. These are going to be sent to a laboratory for processing, whereas antigen tests can be processed anywhere, such as your doctor’s office or even your home. That’s also why antigen tests are commonly referred to as “rapid tests.”
Antibody Tests
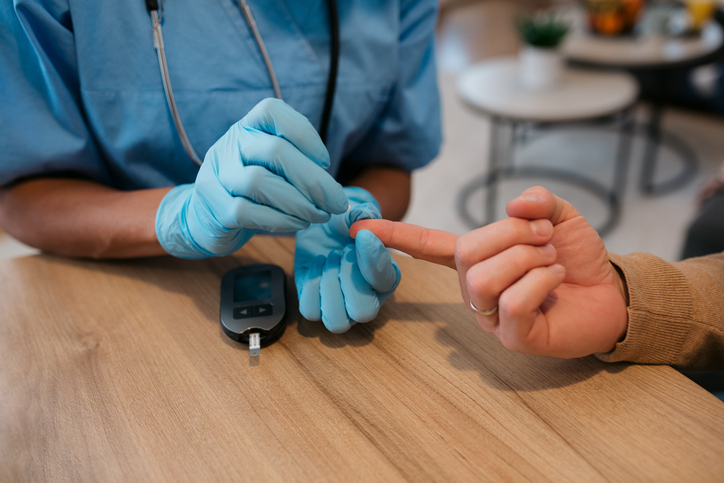
Source: Brothers91 / Getty
An antibody test reveals whether or not a person has had an infection in the past. If someone recovered from a virus at least two to three weeks prior to taking the test, their body would have produced antibodies, which would appear in the test. An antibody test cannot detect if someone currently has COVID-19. Antibody tests are done through a blood test, which is why there are no at-home antibody tests. The blood is either taken from a vein or a fingertip, and results can be available anytime from the same day up to a week after the blood collection. It is worth noting that the medical community debates the usefulness of antibody tests because they can also pick up antibodies from a vaccine, making it difficult to know if a vaccinated person has had COVID-19 in the past.
At-Home Test Mistake #1: Taking It Too Soon

Source: AlexanderFord / Getty
There are many factors that determine whether or not you need to get tested after exposure, and how long to wait. The CDC lays them out here, and they are different for those who are boosted, received their primary vaccinations but no booster or have had no vaccines at all. Overall, the guidelines point to getting tested five days after exposure, but sooner if you start experiencing symptoms. So with that in mind, if you spend time with a friend on a Monday who calls you Tuesday to say she’s tested positive for COVID-19, do not take your test yet. It is too soon after the exposure for a test to detect the infection, so it would be a waste of the test.
At-Home Test Mistake #2: Being Too Gentle

Source: Grace Cary / Getty
While being able to test at home is convenient, there’s value in having a professional take your sample. Most are familiar at this point with the stinging sensation of a nose swab. And most wouldn’t subject themselves to that feeling. It’s in your nature to avoid pain, so when you start to feel discomfort from an at-home test, you might pull back and fail to apply enough pressure to collect a viable sample. If you do not insert the swab far enough, do not apply enough pressure or do not circle the swab long enough, you might not get a viable sample.
At-Home Test Mistake #3: Ignoring Symptoms

Source: DjelicS / Getty
A negative test result should not be the only factor driving your decision-making. If you have symptoms of any kind such as a runny nose, sore throat, cough or headache, a negative test isn’t your green light to go out and be with others. You might have received a false negative. Or, you might simply have something else that is contagious like the flu or a cold. Only a negative test combined with an absence of symptoms should be your greenlight to be around others. And do keep in mind that if you live with someone who has COVID-19, the most responsible thing to do is quarantine – no matter what your test says. Living with an infected individual puts you at risk of contracting the virus at any time, so false negatives become highly likely in that scenario.
At-Home Test Mistake #4: Hoarding Tests

Source: SOPA Images / Getty
First it was toilet paper; now it’s COVID-19 tests. We’re talking about hoarding. There are many reasons to hoard tests – like panic, or a desire to stay social – but none of them are good enough reasons to deprive others of tests. CNN reports that the hoarding has gotten so bad that Amazon, Walmart and certain pharmacies have started limiting the number of at-home tests per customer. Remember that when you hoard tests so that you can go on that ski trip or go to that concert, you could be depriving people of tests who need them to go to their work or send their children to school.












