What A Placenta Previa Diagnosis Means For Your Pregnancy
Share the post
Share this link via
Or copy link
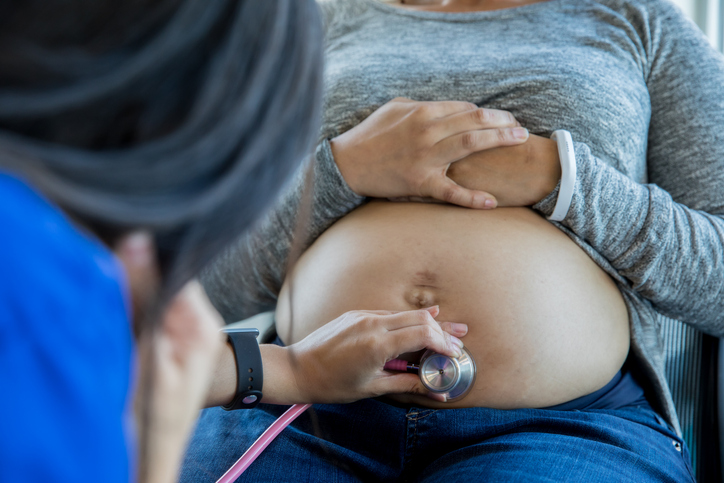
Source: Courtney Hale / Getty
I have a confession to make about my first pregnancy: I wanted a cesarean section almost from the moment I learned I was pregnant. I was never one of those women who felt like experiencing hours of labor and delivery and possible tearing of my reproductive anatomy made me anymore of a mother. I never knocked any woman who desired that experience, or felt cheated if for whatever reason things didn’t go according to plan, but the very thought of painful contractions and pushing through sweat and tears for hours while strangers pried my thighs apart both terrified and exhausted me. I remember thinking that if I had to have a vaginal delivery, I’d push through it (literally) but if for whatever reason having a c-section became a viable option, I’d be relieved and ready for my minor bikini cut across my abdomen as long as my child was safe and healthy.
I managed to have a pretty symptom-free pregnancy before I began to see my OB/GYN more frequently during my second trimester. I hadn’t experienced any morning sickness and besides a little food aversion and fatigue, my baby was doing my body well and developing as expected. But around 20 weeks or so my OB/GYN shared that after an ultrasound, she had some concerns about the placement of my placenta. The blood-rich organ that feeds the baby nutrients and oxygen was sitting low in my uterus and I was officially diagnosed with placenta previa. The good news? The placenta wasn’t actually covering the cervix The bad news? It was sitting too close for my doctor’s comfort, which was technically considered “partial previa.” She advised the next steps would be to monitor the situation and hope the placenta shifted itself in the next few weeks. Several weeks and two very uncomfortable transvaginal ultrasounds later however, it appeared my placenta had set up shop and no plans on relocating.
Around 32 weeks, my OB/GYN made the recommendation to plan for a scheduled c-section. According to her measurements, my placenta didn’t appear to be a barrier to safe vaginal delivery at the time, but ultrasounds can be off slightly and the labor and delivery was “no place to be a cowboy.” A scheduled c-section would allow her time to assess the situation once she could take a closer look at my stubborn placenta, instead of the alternative: risking going into labor and having an emergency c-section if they discovered the placenta was closer than predicted and risk rupturing and hemorrhaging, a dangerous situation for both me and baby.
Love MadameNoire? Get more! Join the MadameNoire Newsletter
We care about your data. See our privacy policy.
Thinking back, I can still picture my doctor bracing herself for the tears and guilt that can come with expectant mothers who might be disappointed at the lost opportunity to experience a vaginal birth. But honestly, I was relieved more than anything and just wanted the healthiest pregnancy possible. However, for the remaining few weeks of my pregnancy, there were some limitations. I was now considered high-risk with the goal being making it to my scheduled C-section at 37 weeks without going into labor. Placenta previa can be a big deal and impact your pregnancy in many ways. Here are a few things you can expect if you’re facing diagnosis:

Source: JGI/Jamie Grill / Getty
You probably didn’t do anything to cause it.
Smoking, increased age and previous c-sections are a few risk factors associated with placenta previa, but overall doctors are unsure exactly what causes the condition. According to the American Pregnancy Association about 1 in 200 women will experience a placenta previa that doesn’t correct itself by the third trimester.

Source: Jose Luis Pelaez / Getty
The problem may fix itself.
A placenta previa detected in the first trimester has up to a 90 percent chance of moving on its own; as the uterus grows, the placenta can shift along with it. However, until it actually does move a diagnosis is still serious, with providers advising expectant mothers to avoid activity that can cause trauma or irritation to the placenta.

Source: JGI/Tom Grill / Getty
You may experience bleeding or contractions.
Some women aren’t even aware they have placenta previa until it’s detected on an ultrasound. However, a significant number endure painless bleeding, and some may even experience contractions which may risk tearing of the placenta. Women who experience bleeding during pregnancy, specifically in addition to a placenta previa diagnosis should consult their prenatal provider. Significant bleeding may require emergency assistance.

Source: Jose Luis Pelaez Inc / Getty
You may eventually be scheduled for a c-section.
My OB/GYN allowed me to get up to 32 weeks of pregnancy before she made the judgment that it was unlikely my placenta would be budging. Ironically, my daughter had turned and was in the right position for a vaginal delivery at that point, but with the previa diagnosis the goal was to make it to 37 weeks for a scheduled C-section. Contractions can be dangerous when paired with a placenta previa diagnosis since the dilation of the cervix can cause the placenta membrane to tear and hemorrhage. About 75 percent of women with placenta previa in the third trimester deliver via C-section before labor starts.

Source: sturti / Getty
C-sections may increase your risk of developing placenta previa in future pregnancies.
Scar tissue in the uterus can increase the risk of placenta previa, so although a c-section is typically necessary for a safe delivery it can also increase your chances of developing placenta previa in future pregnancies. Fibroid removal and dilation and curettage (D&C) are other procedures that increase the risk of placenta previa.

Source: KidStock / Getty
You’ll get super familiar with transvaginal ultrasounds.
During my initial diagnosis, my OB/GYN scheduled me to have two transvaginal ultrasounds to get a better picture of what was going down in my vaginal canal and my cervix. This type of ultrasound requires a wand-like instrument being inserted into the vagina, and is performed with the intention of not disrupting the placenta to avoid any bleeding. However, it wasn’t about getting cute pics of my child sucking her thumb as much as it was being uncomfortable laying flat with a whole human bearing down on my back. Luckily, the procedure doesn’t last long but make sure to let your provider know if you’re experiencing any pain.

Source: Monkey Business Images / Getty
Penetration will be paused.
I had a whole wedding and honeymoon at the beginning of my third trimester. Clearly we got an early start on consummating the marriage, but while under normal circumstances sex is completely safe and even encouraged during pregnancy, penetration or anything that could cause trauma to the placenta is discouraged. This includes orgasms even without the help of your partner, so you’ll be breaking up with your vibrator as well.

Source: Artem Varnitsin / EyeEm / Getty
You’ll be advised to lay low.
I was never placed on bed rest since I had a pretty healthy pregnancy outside of my partial placenta previa, but in addition to sex any vigorous activities were off limits. If you’ve been diagnosed with placenta previa, your doc may tell you to save the yoga and cardio for after your delivery.

Source: BSIP/UIG / Getty
Your IUD may also be to blame.
No birth control is 100% and while IUDs are extremely effective at pregnancy prevention, when a pregnancy does occur with an IUD in place, it can be a tricky situation to navigate. Resolutions in these situations are typically handled on a case by case basis, with many medical providers choosing to leave the IUD in place if removal appears harmful to the pregnancy. But is some situations that decision can have lasting effects, such as this case in which a provider assessed scarring from an IUD lead to placenta previa and an emergency hysterectomy.
Toya Sharee is a sexual health expert who has a passion for helping young women build their self-esteem and make well-informed choices about their sexual health. She also advocates for women’s reproductive rights and blogs about everything #BlackGirlMagic and #BlackBoyJoy. Follow her on Twitter @TheTrueTSharee or visit her blog, Bullets and Blessings.
Related Tags
pregnancy complications











