NEC: Living With A Neonatal Illness And Fighting To Stay Alive
SUNDAY NOIRE: I Came Into This World Fighting To Stay Alive

H. Armstrong Roberts/ClassicStock
Every year in the U.S., thousands of babies develop necrotizing enterocolitis (NEC) and hundreds of these babies die after their NEC diagnosis. NEC is an intestinal disease that primarily causes an inflammatory process that can lead to intestinal tissue damage for premature and fragile infants. Many babies who develop NEC are left with lifelong complications, and tragically, some die from the disease. Surgical NEC survival rates are improving, but according to the C.D.C., NEC is still a leading cause of illness and death among preterm infants in the United States. About 5 to 12 percent of infants born at very low birth weight (less than 1500 grams) are diagnosed with NEC, while preterm or low birth weight are at an increased risk. NEC is one of the leading causes of illness and death among preterm infants and the leading cause of death due to gastrointestinal disease among preterm infants.
Although NEC is not rare in the neonatal intensive care unit, NEC is an overall rare disease in the U.S. population, affecting less than 200,000 people. Too many families learn about NEC for the first time when their child is being diagnosed, which leaves families feeling isolated. For Black families who are navigating racism in the hospital setting along with a diagnosis of a rare and quickly progressing disease, feelings of distrust are only exacerbated. Similar to other health disparities observed in birth outcomes, NEC disproportionately impacts Black infants. This bias is observed even when the data accounts for socioeconomic differences.
Linseigh Green is a NEC survivor, activist, and NEC community advocate. She is sharing her story to help others understand this rare disease and bring attention to the challenges of living with an invisible disability. The National Birth Equity Collaborative and Linseigh are bringing attention to NEC and its disproportionate impact on Black families. Linseighis an audio artist, writer, vocalist, actress, and rare disease advocate who earned degrees at the University of Cambridge (MSt Creative Writing); NYU Gallatin School of Individualized Study (BA Social Impact Storytelling); and Royal Holloway/Story Futures (MA Immersive Storytelling).
BIRTH STORY
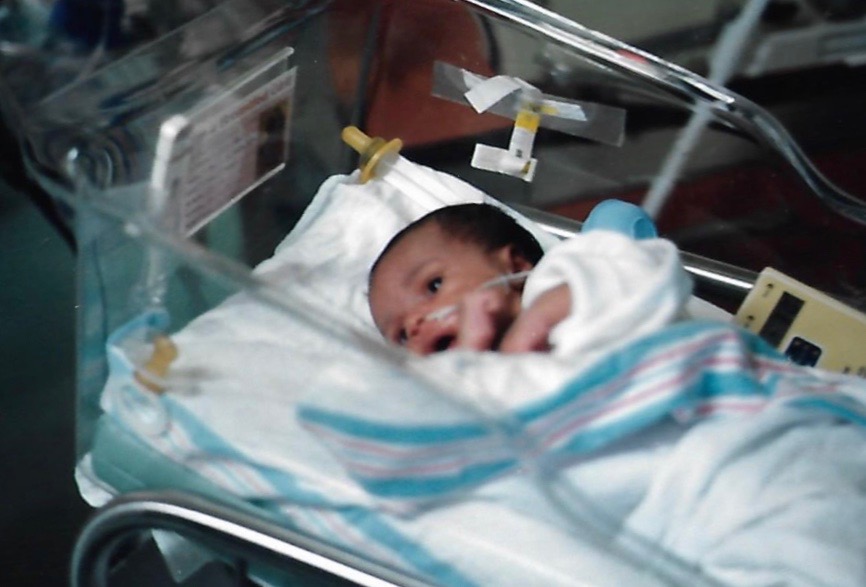
Source: Courtesy of Linseigh Green / Linseigh Green
I came into this life fighting to live. I’ve never stopped. Though I was born full term, I had stopped growing after five months in the womb. I was sent to the NICU before my parents could hold me. They watched through a window as I repeatedly failed to keep my mother’s milk down. My stomach was swollen, but it wasn’t from food.
NEC DIAGNOSIS
An investigation revealed that I was suffering from necrotizing enterocolitis (NEC), but my care team, despite my parents’ pleas, wouldn’t elaborate. It was 1997 and Google was only a dream. The library was useless; friends hadn’t experienced it. Finally, the nurse offered them a book on preemies with a paragraph on NEC, instructing my parents not to read beyond a certain line. It said I had a neonatal intestinal disease; essentially, part of my bowel was “dying.” When they read past the dictated line (you knew they were going to), the forbidden text continued: I likely wouldn’t survive. If I did, by the age of seven, it would become clear I’d never succeed in school.
SURVIVING NEC

Source: Courtesy of Linseigh Green / Linseigh Green
I survived thanks to an operation in which the “bad” part of my colon was removed. My childhood was mostly normal, except my gross motor skills were poor and I couldn’t eat normal amounts of food. My mom, a schoolteacher, showered me with workbooks until, at the age of seven, I was ahead in most subjects (despite my slow pacing). I recently graduated from Cambridge with distinction, and have just completed my third degree, despite being diagnosed with cognitive dysfunction. But there were some things we weren’t warned about: at sixteen, an occasional searing pain around my surgical scar had escalated into uncontrollable shaking, blackouts and vomiting. I was told I was suffering from long term complications of NEC.
These episodes, which required hospitalization and almost called for surgery, recurred annually. My doctors were always confused, but they were certain my condition was unrelated to NEC. I was berated for eating too many burgers; denied care until I confessed to substance abuse or alcohol poisoning; locked in an office until I admitted I was pregnant. I’ve had such traumatizing experiences, I nearly dropped out of university. I now have PTSD, yet I’m still trying to find follow-up care, because I believe in my right to a future. Now that I, not unlike other NEC survivors, have developed cognitive issues, I’m terrified of what this means for my perceived competence and medical autonomy — despite being an adult with three degrees, I am already treated as a poorly behaved child.
LIVING AS A SURVIVOR OF NEC

Source: Courtesy of Linseigh Green / Linseigh Green
A few months ago, my mom realized I was inheriting her experience with my disease. Before sharing my diagnosis, a nurse demanded to know what she had done wrong: had she used substances while she was pregnant? Did she drink alcohol? Was she being honest about me being an IVF baby? That healthcare would sooner harass or criminalize me than offer help is merely a rite of passage.
Linseigh’s care team’s refusal to thoroughly communicate with her parents may sound familiar, as it is symptomatic of the prevalence of racial bias in the NICU. As gatekeepers of knowledge, healthcare providers may withhold information about one’s baby — a Black mom may be perceived as less competent, educated, responsible, or credible than their white counterparts. Bias and bigotry may also result in judgmental or neglectful treatment.
Many mothers and birthing people are unacceptably blamed by medical professionals and society for their children’s health conditions. This experience is referred to as “mother blame.” Unlike Linseigh’s family, we now have access to a wealth of information online — the NEC Society, for instance, has educational resources that can help families make informed decisions, advocate for themselves, and find answers they may not otherwise be given.
The information is out there, but is it making its way into the hands of Black families? The NEC Society’s Outreach Coordinator, Linseigh is working hard to increase equitable access to information by leading the organization’s online community, helping patient-families share their stories, and serving as the first point of contact for many who have been affected by NEC. Despite the disease disproportionately affecting Black infants, the leaders in the NEC community are overwhelmingly white.
A NEC survivor also told Linseigh that she wouldn’t be accepted as her authentic self in a mostly white space. When Linseigh mentioned this to her mother, she responded: considering her experience with healthcare (and society as a whole), how could she expect people to care about the trauma she has been through as a Black woman? Unlike white women, she did not assume others would listen and empathize with her story.
The NEC Society is working to engage and elevate Black voices and leadership, but this key perspective is currently missing in the neonatal community, leaving only a perceived white default to inform solutions and shape discourse. It is important to shift the conversation from mother blaming and bias to creating environments where empathy, equity, and quality health care are prioritized.
To authentically collaborate with Black NICU families, we need to raise the profile of NEC in our own communities with a coordinated effort. We can raise awareness about not only the disease, but also about how we can circumnavigate knowledge gatekeeping in healthcare. Let’s discuss NEC in our communities, partner with organizations that center the experiences of Black NICU families, and promote education on respectful maternity care to medical professionals.
RELATED CONTENT: Baby Formula Recall Brings Attention To Rare But Serious Cronobacter Infection












